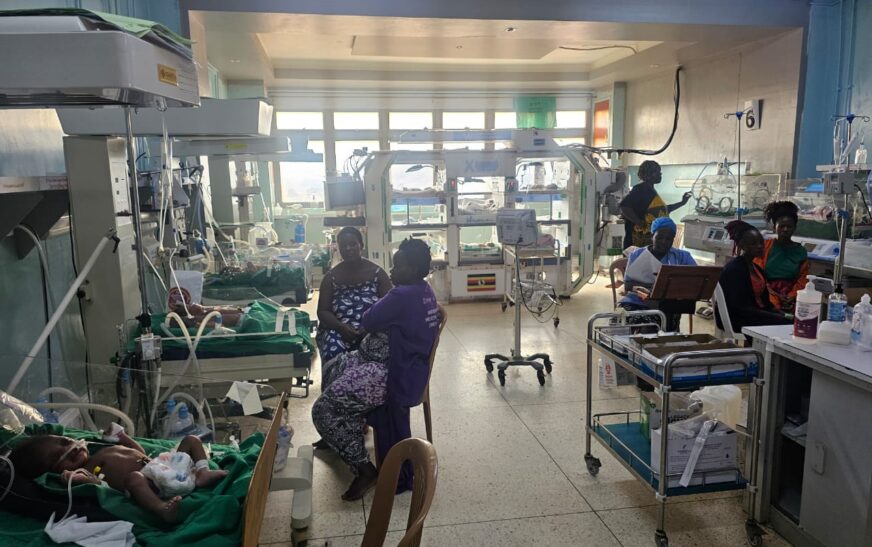
Every week, Isabelle Furaha leads a dedicated team of volunteers moving between hospital wards and homes across Uganda, following up on some of the country’s most vulnerable lives premature babies who have survived birth but remain at high risk.
Under her leadership, the team equips mothers with essential skills to care for their infants, including how to keep them warm, ensure proper feeding, and detect early signs of infection. In many cases, these interventions mean the difference between life and death.
Furaha is the founder of Mama Tulia Ministries, an initiative focused on supporting mothers and newborns during the critical transition from hospital to home.

Her impact has now earned global recognition. This week, she received the Innovation and Collaboration Award at the Global Foundation for Care of Newborn Summit in Germany.
Despite the recognition, Furaha attributes the success to collective effort.
“Our work has always been about collaboration,” she said. “From our staff to volunteers and partners, this recognition belongs to everyone supporting these families.”
In Uganda, many premature babies survive neonatal intensive care but face significant risks after discharge. Infection, poor home environments, and limited caregiver knowledge continue to threaten their survival gaps Furaha set out to address through a continuum-of-care model.
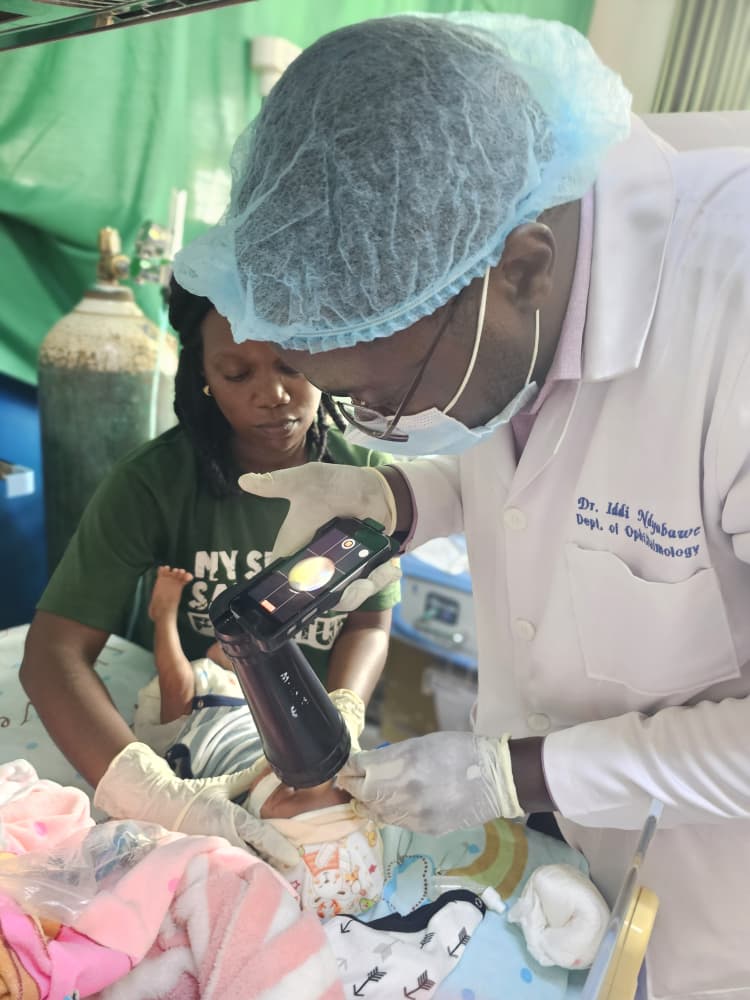
Through Mama Tulia Ministries, mothers receive support before discharge, followed by regular home visits and access to specialised interventions such as screening and treatment for Retinopathy of Prematurity, a condition that can lead to blindness if not detected early.
Over the years, Furaha’s model has reached more than 10,700 mothers and babies, conducted over 7,600 home visits, and strengthened care through more than 500 hospital engagements.
The impact is particularly notable in ROP care, where over 2,000 babies have been screened. Of these, 262 were diagnosed and 243 successfully treated—preventing avoidable blindness.
Earlier this year, Furaha expanded the initiative with the launch of the Tulia Tender Nest Transition Home, a facility designed to stabilise high-risk mothers and babies before they return to their communities. Since February, it has supported more than 20 mothers and 24 babies.

Beyond medical care, her work also addresses the social challenges affecting newborn survival. The organisation has distributed over 200 water filters to vulnerable households and provides psychosocial support, including programmes for teenage mothers and initiatives that encourage fathers to take part in newborn care.
Health experts say such integrated, community-based approaches are essential for improving outcomes for preterm babies, especially in low-resource settings where post-hospital care remains limited.